
If you have diabetes, also known as diabetes mellitus, you would be aware of the various complications that diabetes can cause, such as damage to the eyes, kidneys, and heart. However, there is one more risk to consider: your likelihood of developing bone illnesses. Persons with type 1 and type 2 diabetes have a greater risk of fractures, especially hip fractures, than people without diabetes.
Although the link between diabetes and an increased risk of bone disorders and fractures is not completely understood, researchers agree that there are specific steps that can be taken to reduce the risk.
Bone Problems associated with Diabetes
Any disorder that damages the skeleton and makes the bones fragile and susceptible to fractures is known as bone disease (bone breaks). Fractures and weak bones are not a typical aspect of growing older. While the development of healthy bones begins in childhood, anyone of any age can benefit from better bone health.
Osteoporosis, osteopenia, Charcot foot, diabetic hand syndrome, diffuse idiopathic skeletal hyperostosis, frozen shoulder, and Dupuytren’s contracture are all bone ailments linked to diabetes.
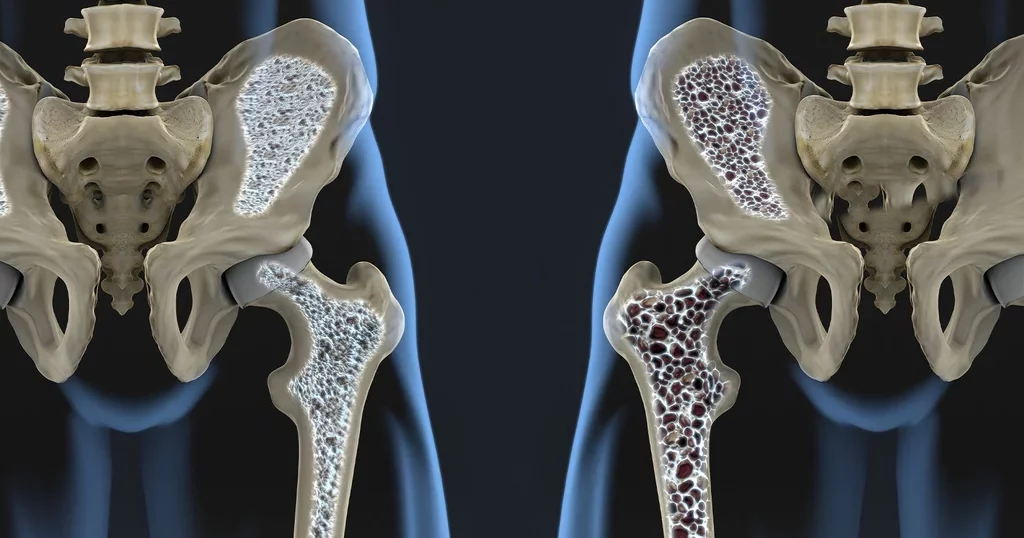
1. Osteoporosis
Osteoporosis, defined by decreased bone mass and structural degradation of bone components, is one of the most frequent bone illnesses. It can cause bone instability and raise the risk of hip, wrist, knee, and spine fractures. Although osteoporosis is preventable and treated, it affects a large number of people as they get older. Osteoporotic fractures affect one in every three women over 50 and one in every five men over 50 around the world. Low bone density is linked to osteoporosis, which is caused by the loss of essential minerals, mainly calcium, in the bones. Bones become weak and fracture readily as a result of this loss. People with diabetes have poorer bone quality, which puts them at risk for osteoporosis. For more details, see Osteoporosis.
2. Osteopenia
Bones with osteopenia are weaker than typical. Bone mass and density, on the other hand, are not low enough to cause bones to break readily. Osteopenia is a condition that falls between between strong, healthy bones and osteoporosis.
According to research, osteopenia is a well-known consequence of Type 1 Diabetes, particularly in those who take high insulin doses.
3. Charcot Foot
Charcot foot, also known as Charcot neuropathic osteoarthropathy, is a diabetic condition that produces foot and ankle abnormalities. Swelling, redness, and apparent deformity are some of the symptoms. 3
Assistive devices (to relieve pressure on the afflicted joint) and tailored shoes are two treatments for Charcot foot (to allow the joint to heal). When all other alternatives have failed, surgery is considered.
4. Diabetic Hand Syndrome
Diabetic hand syndrome, also known as diabetic cheiroarthropathy, is a type 1 and type 2 diabetes condition in which finger movement is restricted and the hands become waxy and heavy. Diabetic hand syndrome is more likely in persons who have uncontrolled diabetes for a long time.
5. Diffuse Idiopathic Skeletal Hyperostosis
Diffuse idiopathic skeletal hyperostosis (DISH) also known as Forestier disease, is a kind of arthritis that affects tendons and ligaments, primarily in the spine. DISH induces calcification (hardening) of tissues and the formation of bone spurs in places of the spine that connect to bone.
DISH can also cause calcification of bones throughout the body, as well as bone spurs in the hips, knees, shoulders, hands, and feet. This condition can be caused by Type 2 Diabetes or any other disorder that elevates insulin levels.
6. Frozen Shoulder
Frozen shoulder, occurs when the ligaments that surround the shoulder become inflamed and rigid. Inflammation and diabetes make ordinary healing more difficult, causing the shoulder joint to stiffen to the point where even simple tasks like buttoning a shirt become difficult.
Frozen shoulder is a painful ailment that can last for months or even years. Physical therapy, anti-inflammatory medications, and corticosteroid injections are used to treat it. According to research, those with uncontrolled diabetes are five times more likely to have frozen shoulder than those who do not have diabetes.

7. Dupuytren's Contracture
Dupuytren’s contracture, also known as palmar fascia, is a hand ailment in which the connective tissues beneath the skin of the hand gradually thicken and scar. While the condition isn’t usually unpleasant, it does limit finger movement and can cause them to curl and bend towards the palm.
Diabetes is a risk factor, and diabetics are 3 times more likely to develop Dupuytren’s disease. Dupuytren’s contracture is most common in those with T1D.
How to prevent bone problems in Diabetes?
Regular exercise, a balanced diet, and healthy lifestyle choices are the greatest methods to sustain bone health for everyone, including persons with diabetes.

A. Regular Exercise
Exercise strengthens your bones, which benefits your musculoskeletal system. Weight-bearing and strength-training workouts are the best activities for bone health.
Jogging, stair climbing, walking, dancing, yard labor, and tennis are all weight-bearing exercises. If you can manage strength-bearing exercises like lifting weights and doing push-ups, you can help strengthen your bones while simultaneously improving your balance. See 5 min Tai-chi exercise for joint pain
B. Healthy Diet
Fruits and vegetables, lean meats and fish, whole grains, nuts and seeds, nonfat and low-fat dairy products, and other calcium-rich foods are all part of a daily balanced diet. Make sure you’re receiving enough vitamin D and calcium to keep your bones healthy. Click here to see 10 healthy foods for good bone health.

C. Lifestyle Changes
Both smoking and drinking are detrimental to one’s bones. Women who smoke are more likely to reach menopause earlier, which means they are more likely to experience bone loss owing to lower oestrogen levels. Because those who drink heavily have poor nutrition and are more likely to fall, alcohol can cause bone loss and fractures.
A word From Sundarspine.com
Having diabetes does not automatically predispose you to bone damage. If you have other risk factors, such as a family history of bone problems, speak with your healthcare practitioner as soon as possible so that you may work together to prevent and detect bone problems before they worsen.
If you notice swelling, redness, numbness, or pain in your bones, muscles, or joints, contact your doctor. These signs and symptoms must be handled as soon as feasible.
While there are no cures for many bone illnesses, therapies can help to lessen pain, swelling, stiffness, and other symptoms, as well as the risk of deformity and disability. Despite having diabetes and bone difficulties, most people can have a decent quality of life and a positive outlook.
